(NEW YORK) — At least two Americans have died and 17 have suspected or probable cases of a potentially deadly infection linked to an outbreak at cosmetic surgery clinics in Mexico.
The infected patients contracted fungal meningitis after having procedures under epidural anesthesia in Matamoros, Mexico — just across the border from Brownsville, Texas — according to the state’s Department of Health Services.
More than 200 people across the U.S. who underwent operations between Jan. 1 and May 13 of this year may be at risk, according to the Centers for Disease Control and Prevention.
Despite the closure of River Side Surgical Center and K3 Clinica, people developed symptoms of fungal meningitis weeks later.
Here are the signs to look for and how the infection can be treated before it’s too late:
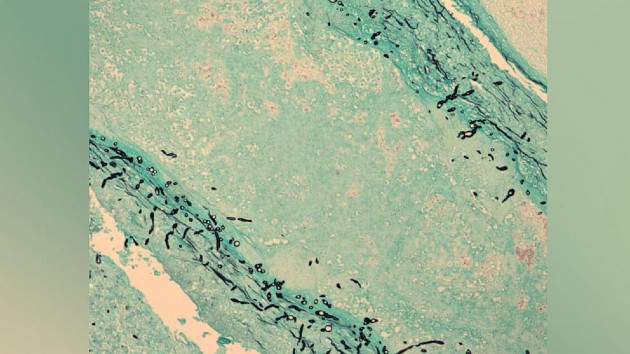
What is fungal meningitis?
Meningitis is a type of infection and inflammation affecting the fluid and three meninges — or membranes — that protect the brain and spinal cord.
Fungal meningitis specifically occurs after someone contracts a fungal infection that spreads to the brain or spinal cord, according to the CDC.
Signs and symptoms can appear weeks after initially developing the infection and include headache, fever, nausea, vomiting, stiff neck, sensitivity to light and an altered mental state.
How do people contract fungal meningitis?
Many fungi are too small to see with the naked eye so it’s easy for people to breathe in or ingest microscopic spores, the CDC says.
Fungal meningitis is not contagious and cannot spread from person to person.
“While rare, outbreaks of fungal meningitis following medical and surgical procedures have occurred,” the CDC says on its website. “Healthcare providers can find information on testing and treatment options for patients with suspected or confirmed fungal meningitis. These options are applicable to patients regardless of where exposure occurred.”
How is fungal meningitis treated?
To be diagnosed with fungal meningitis, a patient gives samples of blood or cerebrospinal fluid that are tested for the presence of fungi.
If results are positive, patients are then given high doses of antifungal medications intravenously, according to the CDC, which may include amphotericin B — a medication that stops the growth of fungi.
Next, patients are given antifungal medications by mouth, the health agency said, which may include itraconazole or fluconazole.
There is no specific timeline for how long a patient takes these medications; it will depend on the patient’s immune system. For example, those with underlying conditions weakening the ability of the body to fight infections, including cancer or HIV/AIDS, may have a longer course of treatment.
Is fungal meningitis deadly?
There is no data on the number of deaths per year from fungal meningitis but public health experts say it can turn deadly if not identified and treated quickly.
A 2017 study on an outbreak in Virginia found that 9.678% of the people who developed fungal meningitis died even after receiving treatment and 100% with fungal meningitis who did not receive treatment died.
One of the two patients who died in this current outbreak is Shyanne Medrano, a 31-year-old mother from Houston, according to local ABC affiliate KRGV-TV.
She began to feel sick not long after visiting K3 Clinica in March to receive a Brazilian butt lift.
Weeks later, Medrano was admitted to a hospital with symptoms of the infection. She later developed a blood clot, a family member told KRGV. On May 16, two months after the procedure, Medrano died.
Can I prevent fungal meningitis?
There are no vaccines that protect against fungal meningitis. The CDC does recommend several prevention measures.
These include avoiding areas that contain a lot of dust, staying inside during dust storms, avoiding activities that involve close contact to dirt and cleaning skin injuries with warm water and soap to avoid the odds of developing an infection.
Copyright © 2023, ABC Audio. All rights reserved.